Irritable bowel syndrome (IBS) is a digestive disorder that affects about 20% of people around the world. It’s the most common gastrointestinal diagnosis and the second most common cause of absence from work.
‘IBS is a chronic condition that you’ll need to manage long term,’ says Dr Roshaan Saloojee, a Livi GP. ‘Although it doesn’t lead to severe disease, it can have a big impact on your everyday life, so finding ways to manage it is key.’
While the cause of IBS remains unclear, it’s widely accepted that there is a strong link between gut health and mental health, as a result of what’s known as the gut-brain axis. By learning to manage your anxiety and stress levels, you may be able to minimise your IBS symptoms too.
What causes IBS, and who is likely to have it?
‘The exact cause of IBS is unknown, but possible causes include over-sensitive nerves in the gut or immune system, food passing through the gut too quickly or too slowly, stress, or a family history of IBS,’ explains Dr Saloojee.
‘Post-infectious IBS is caused by a previous bacterial infection in the gut, which can then lead to the syndrome.’
You’re more likely to have IBS if:
- You’re under 50 years of age
- You’re female
- You have a family history of IBS
- You have a history of anxiety, depression or other mental health problems
What are the most common IBS symptoms?
Common IBS symptoms include:
- Cramping
- Abdominal pain
- Bloating
- Gas
- Diarrhoea and/or constipation
‘Symptoms tend to come and go,’ says Dr Saloojee. ‘They can last days, weeks or months and can vary in severity.’
What’s the connection between our gut and our mind?
The link between the brain and the gut is strong, and virtually every gut function is sensitive to stress. Most of us are familiar with the gut’s reactions to different emotional and psychological experiences – think about the expression ‘butterflies in the stomach.’
This is because of the gut-brain axis. ‘The brain and nerves that control your body are called the central nervous system, which is divided into 2 parts: the sympathetic and the parasympathetic nervous systems. Some say there’s a third part called the enteric system, which controls the gut,’ Dr Saloojee explains.
‘The gut-brain axis is a term used to describe the two-way communication between the central and enteric nervous systems, linking the emotional centres of the brain with the functioning of the gut.’
Because of the gut-brain axis, emotions can impact the gut in a number of ways, and the gut can influence your mental state too.
That’s not to say that all gut symptoms linked to mental health are due to IBS. Anxiety, for instance, is known to cause everything from stomach aches to a change in bowel movements.
Can stress and anxiety cause stomach pain and IBS?
‘If you have IBS, the balance between the brain and the gut is disturbed,’ says Dr Saloojee. ‘Stress and anxiety can activate the central nervous system, which in turn releases hormones that affect digestive processes in your gut and may cause diarrhoea, constipation, gas or discomfort.’
The link between the brain and the gut is thought to play a key role in IBS
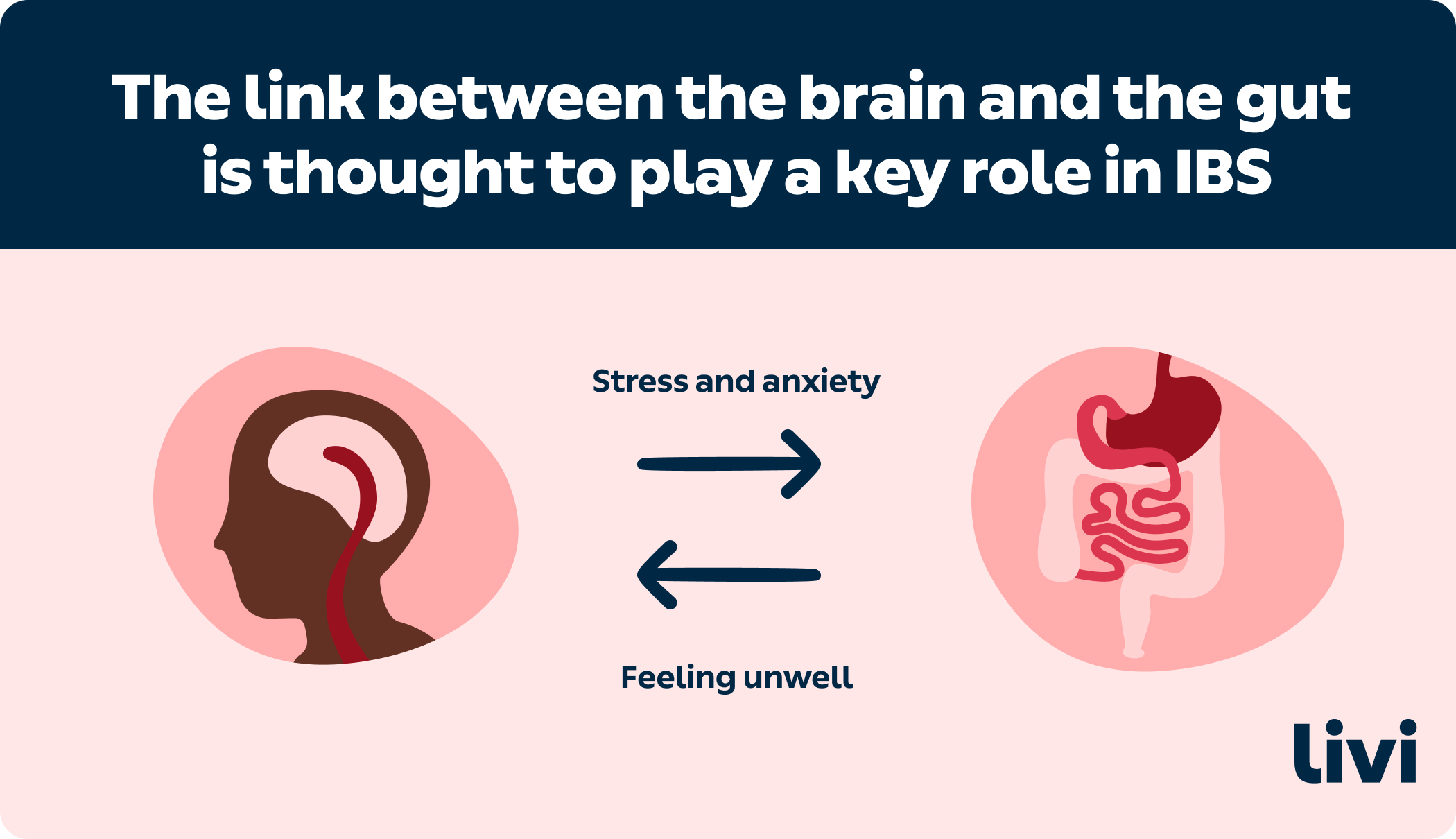
Increasingly, IBS is becoming known as a condition of both irritable bowel and irritable brain. In addition to stress and anxiety triggering IBS symptoms, IBS can trigger stress and anxiety, causing a vicious cycle. A survey of IBS patients found that 44% also suffered from anxiety, with 84% suffering from depression.
‘While the link between stress and IBS is clear, stress is usually not the only influence,’ says Dr Saloojee. But it can play a central role. ‘Stress releases hormones that can negatively impact the gut,’ she says. ‘Chronic stress can cause an imbalance of the gut’s bacteria and be a key factor in a person developing IBS.’
Stress and major life traumas are known to worsen IBS symptoms. Many people experience spikes in their stress levels just before they start getting IBS symptoms. In fact, some researchers argue that it’s nearly impossible to improve IBS without first addressing stress. ‘This is why treating IBS in a holistic way is so important,’ says Dr Saloojee.
How is IBS treated in the context of anxiety and stress?
‘Some people can control their IBS symptoms by managing diet, lifestyle and stress,’ says Dr Saloojee. But when simple lifestyle changes aren’t enough, a combination of medication and counselling can help.
‘The psychological treatments for IBS with the strongest evidence are CBT, hypnosis and mindfulness,’ adds Dr Saloojee. ‘CBT teaches you to change unhelpful thinking patterns, engage in relaxation techniques and change behaviours that may contribute to physical and mental illness. Patients learn how the stress response is linked to gut symptoms and how to modify these responses. Research shows that CBT can be effective in improving bowel symptoms, quality of life and reducing stress and anxiety.’
Some researchers believe that IBS patients suffer from heightened gut sensitivity that makes normal gas and bowel movement more painful. That might be why some people with IBS find medicines like antidepressants helpful, as they not only improve mood but may also help reduce hypersensitivity in the gut and pain perception.
How can I manage stress to prevent another IBS flare-up?
Dr Saloojee recommends identifying the key stressors in your life. ‘It may be helpful to keep a diary of your gut symptoms every day and see if there’s a connection between how you’re feeling mentally and a flare-up of IBS symptoms,’ she says.
‘Once you’ve identified your triggers, you can take steps towards trying to eliminate or manage them. Because of the link between the brain and gut, this may lead to an improvement in IBS symptoms or fewer flare-ups.’
Dr Saloojee’s tips for reducing symptoms are:
- Try stress-reducing activities, like yoga, meditation, breathing exercises and regular exercise
- Practise good sleep hygiene by going to bed at a regular time, reducing screen time before bed and keeping your room dark
- Get at least 7-8 hours of sleep per night
- Drink at least 8 glasses of water a day
- Cut down on caffeine, which stimulates the gut
- Eat smaller meals
- Avoid fried or fatty foods
- Avoid foods that are known triggers for you – this might include dairy, beans, lentils, cabbage, broccoli or other gas-producing foods
- Try probiotics (good bacteria), which may relieve gas and bloating
- Try increasing fibre in your diet
- Join an IBS support group
- Take symptom-relieving medication if you need it
- Talk to a GP for further support
When should I speak to a doctor about stress and IBS symptoms?
‘If you have IBS symptoms and they’re interfering with your daily life, you should see a doctor,’ says Dr Saloojee.
‘They will take a history of your symptoms and examine you, and they may arrange some blood tests or a stool test. There isn’t a specific test to diagnose IBS, but these investigations can rule out other bowel problems like inflammatory bowel disease, bowel infections, coeliac disease and bowel cancer.’
There are some symptoms you should never ignore:
- Unintentional weight loss
- Bleeding from your bottom or bloody diarrhoea
- A hard lump or swelling in your stomach
- Shortness of breath, palpitations and pale skin (signs of anaemia)
If you’re experiencing any of these symptoms, they could be a sign of something more serious, so you should see a doctor urgently.
If you’re struggling with stress, anxiety or IBS symptoms, try talking to your friends and family, and see a doctor who can help and refer you for further support.
This article has been medically approved by Dr Roshaan Saloojee, a Livi GP.